FNP pass rates drop for 5th consecutive year
- June 1, 2024
Share:

Pass rates on the most common certification exam for family nurse practitioners decreased for the fifth consecutive year in 2023 — a 13% drop since 2018.
What is behind this downward trend? NP education specialists and faculty consultants cite changing academic delivery models, varying admission requirements, preceptor challenges, and increased patient complexity as four of many contributors. All of these factors can be overcome to produce NP graduates who are better prepared for exam success. This article outlines how.
Facts and figures about the FNP certification exams
Two certification exams are available for FNP candidates, one from the American Academy of Nurse Practitioners Certification Board (AANPCB) and one from the American Nurses Credentialing Center (ANCC).
For many years, the majority of FNP candidates have selected the AANPCB exam. This trend continued in 2023, when 67% (17,362) of candidates took this exam. Thirty-three percent (8,530) took the ANCC exam.
The AANPCB and ANCC exams for FNPs are similar in construction and content, and both confer national certification for family practice. Read about the distinguishing features (chiefly, number of questions and time limit) for each exam here.
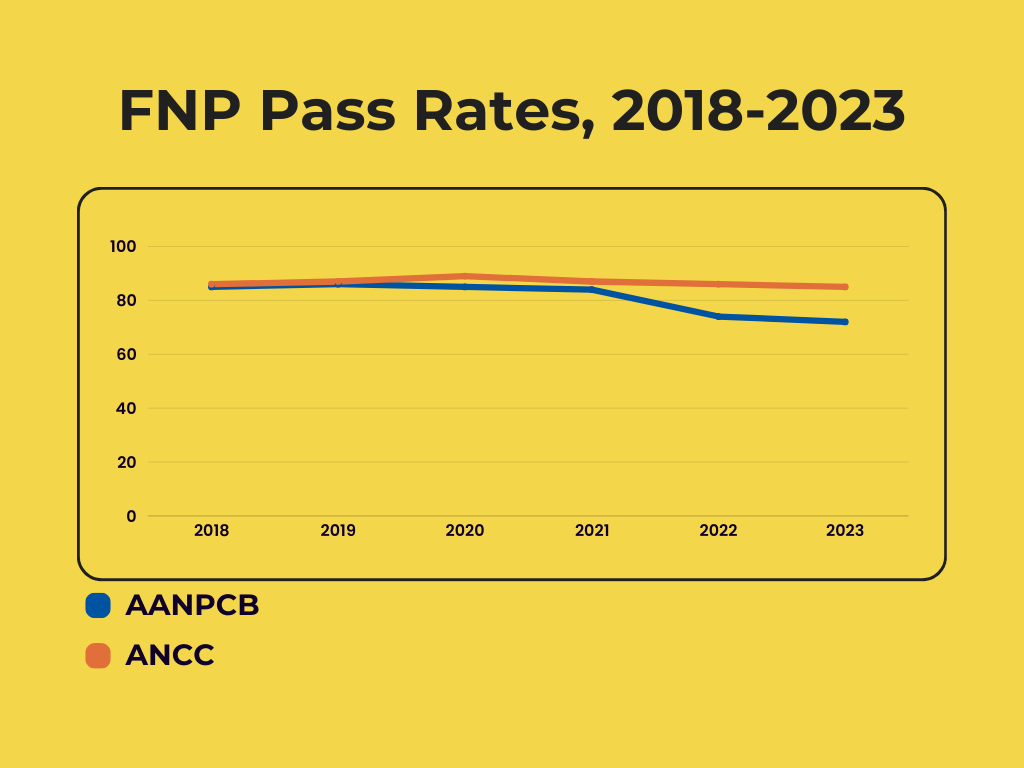
The table below displays trends in FNP pass rates for the past 5 years. The most significant change occurred in 2022, when AANPCB scores dropped 10%. (Read our coverage of that result here.) At the same time, ANCC pass rates have deviated by a much smaller margin. The most significant changes were a 2% increase from 2019 to 2020 and a 2% decrease from 2020 to 2021. AANPCB pass rates declined 13% between 2018 and 2023, while ANCC pass rates declined 1% during the same period.
Academic contributors to declining FNP exam scores
Experts identified Covid-related stressors as a primary influence on the 10% drop in AANPCB pass rates in 2022. Now that the rates have dropped again, it’s time to take a deeper dive, said Kathy Baldridge, DNP, FNP-BC, FAANP, Lead Nurse Practitioner Education Specialist for APEA.
“While the drop in pass rates is concerning, the certification exam is doing what it was designed to do — ensure that a candidate is knowledgeable enough to be deemed competent to practice,” Dr. Baldridge said. Neither the exam content in general, nor the process for certification, have changed in a significant way, she noted. But influential education factors have changed.
Dr. Baldridge and Betty Vicknair, MSN, APRN, PNP, the University and Faculty Consultant and Integration Specialist for APEA, said the growing demand for family nurse practitioners has contributed to changes in admission practices and curriculum design that are affecting student success. They emphasized two concerns in this area:
- The rapid increase in FNP education programs is producing varying admission requirements and education delivery models.
- More students have to find their own preceptors, leading to less continuity in preceptor experiences.
The number of FNP programs is growing in response to national workforce projections. For several years, nurse practitioner has ranked among the top career choices, and in 2024, U.S. News & World Report ranked nurse practitioner as the No. 1 job.
The heightened interest in the NP profession has prompted more universities to establish FNP programs. As these programs work to meet the demands of the market, admission criteria and curriculum delivery are taking new forms. One of the biggest changes has been an increase in virtual programs, and this design is having an impact on student performance.
An analysis of data from universities that administer the APEA Predictor Exam to assess certification readiness found that FNP students in hybrid programs had significantly higher scores on the Predictor Exam — and subsequent success on the certification exam — than students in online programs, Dr. Baldridge said. This analysis found no statistically significant difference in certification results between students in hybrid programs and students in ground programs.
“In discussions with FNP faculty around the country, they’ve expressed a general challenge in the ability to evaluate student competencies in a solely online program,” Dr. Baldridge said. “Consider simulation-based learning. This pedagogical approach to learning is a proven method to bridge the gap between theory and practice. However, when this technique is moved from an in-person to an online system, there are additional challenges to delivering this in a structured manner.
“But it’s not impossible,” she continued. “It will require thinking outside the box in order to evaluate whether learning has occurred and to provide feedback and remediation to the student on a continuum throughout the program.”
In terms of the second education factor — preceptors — this continues be a challenge even though the clinical portion of an NP program is pivotal. Many academic programs require students to find their own preceptors. This means that the depth and quality of clinical experiences can be inconsistent.
“The absolute best student outcomes will come when there is a strong and cohesive relationship between preceptors and faculty,” Dr. Baldridge said. “Strong lines of communication will facilitate the best learning experience and achieved competencies.”
Resources are available from the National Organization of Nurse Practitioner Faculties and other organizations to assist preceptors and faculty in achieving this strong alliance, Dr. Baldridge said.
Preparation contributors to declining FNP scores
Another contributor to declining pass rates for FNP students is preparation, and a particular deficit is the ability to apply critical thinking when answering exam questions.
“In the past few years, there has been an explosion in the number of resources available for NP students to prepare for their certification exams. Not all of them offer a comprehensive approach,” said Lindsey Luther, DNP, APRN, FNP-C, CNE, a Nurse Practitioner Education Specialist for APEA who teaches live review courses and develops study materials.
Another member of the APEA faculty, Nurse Practitioner Education Specialist Jennifer Smith, MSN, APRN, FNP-C, ENP-C, said short-changing the amount of time dedicated to exam prep is also having a negative effect.
“There is substantial data that shows cramming for an exam does not lead to long lasting connections to the information studied,” Smith said. “I would not recommend crash courses in lieu of a comprehensive review.”
Dr. Luther and Smith recommend attending a comprehensive review course and using study materials written and peer-reviewed by NP educators who have clinical experience in NP practice.
“Select a review format that meshes with your learning style, covers the most important material for the exam, and that keeps you engaged,” Dr. Luther said. “Some people learn best using self-paced modules, while others learn best from interactive live courses provided online or in person.”
Based on their experience as faculty members and clinicians, Dr. Luther and Smith cited 5 reasons why students are struggling on certification exams:
- Inadequate exposure to exam-style questions that build critical thinking skills necessary for the exam and for clinical practice
- Weak knowledge in professional issues topics such as scope of practice
- Answering questions based on preceptor experiences (i.e., what they’ve seen during clinicals) rather than evidence-based guidelines
- Increased complexity in patient presentations, requiring higher-level exam questions that graduates aren’t prepared to answer
- Burnout from balancing an NP academic program with a work schedule and/or family needs.
Strategies to improve student performance on certification exams
To address these factors and increase the likelihood of succeeding on the certification exam, Dr. Luther and Smith recommend the following strategies for students:
- Practice answering certification-style practice questions, and do it often. Develop a system for answering these questions efficiently and accurately. (APEA faculty provide guidance for systematically answering certification-style questions during each APEA Live Review Course. Access to exam-style questions is available in MyQBank and the APEA Certification Practice Question Book.)
- Study the conditions most commonly managed in primary care and those that present serious safety issues. “A review course is a great way to quickly review the most common and most important concepts you are likely to see on the certification exam,” Dr. Luther said. “And a Predictor Exam can help you to identify content areas where you have the most to learn.”
- Use a live review course and/or a clinical guideline book as a primary component of study. Stay up to date on guideline changes. Generally, guidelines published 12 months prior to testing are fair game on the exam.
- Master foundational information in the core courses and build strong understanding of the most common patient presentations for your specialty — including more complex conditions.
- Take care of yourself by prioritizing basic needs: sleep, healthy food, exercise, and activities that help you relax.
Strategies for faculty to help students be more successful on certification exams
Academic programs and their faculty also play a role in helping students improve their scores on certification exams. Vicknair, who has been providing support and resources to faculty for almost a decade, emphasized the importance of remediation throughout an academic program.
“Take a proactive approach by assisting students as they progress rather than try to catch up with remedial help later,” Vicknair said. “It’s also important to involve preceptors. They can help students improve their knowledge gaps, oversee assessment skills, and apply pathophysiology and pharmacology knowledge.”
Vicknair also recommends that faculty:
- Consider raising the standards for admission criteria. “Not all students are suitable for an NP program,” she said.
- Start preparing students for the certification exam during their first track-specific theory or clinical course. “Administer assessments to determine if they are prepared to move on,” she recommended.
- Incorporate study questions, case studies, review courses, and simulation into the curriculum.
- Make students more accountable and responsible.
Dr. Baldridge also emphasized the importance of remediation and appropriate assessments.
“Remediation should occur at every level of the program, with a pause until competencies are achieved,” she said. “Through APEA’s research, we have found that students who received remediation in the three core classes of assessment, pharmacology, and pathophysiology had improved scores on the APEA Predictor Exam and higher pass rates on the certification exam.”
The use of valid, reliable assessments should go hand in hand with remediation, Dr. Baldridge said.
“There is evidence of learning when students must prepare for an exam,” she said. “Formative and summative assessments also provide a good measure of knowledge. They identify areas that need remediation and information for curriculum revision.”
In conjunction with these actions, Smith emphasized the need to evaluate students for proficiency in the four domains represented on the certification exams: Assessment, Diagnosis, Planning, and Evaluation.
“Make sure students can apply the content learned in the 3Ps to these domains, both in real-life scenarios and on the exam,” Smith said. “The objective structured clinical examination (OSCE) is often viewed as the gold standard for assessing clinical competencies and should be performed throughout the program to ensure these competencies are met.”